Noticing a hard, tender vein in the leg can be alarming. Many people feel confused when a vein suddenly becomes painful or firm under the skin. Questions arise: Is it just irritation from standing too long, or is it a sign of a more serious problem? When a painful hard vein in leg develops, it’s often difficult to decide whether to monitor it at home, see a primary care doctor, or consult a vein specialist. Understanding what might be happening can help reduce anxiety and guide the next steps for effective care.
What Is a Painful Hard Vein in the Leg?
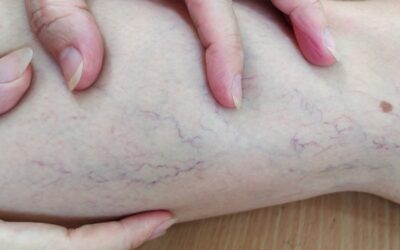
A painful hard vein in leg refers to a vein that feels firm, cord-like, or rope-like and may be tender to the touch. This is usually due to inflammation in the vein wall or a blood clot in superficial veins. Unlike deep vein thrombosis (DVT), which occurs in deeper veins and can be life-threatening, a superficial hard vein is typically less risky but still warrants medical attention.
Common Symptoms of a Hard Vein Under Skin
-
Firm or cord-like vein visible or palpable under the skin
-
Localized pain or tenderness along the vein
-
Redness or warmth over the affected area
-
Swelling in the surrounding tissue
-
Mild itching or irritation
Recognizing these symptoms early can help prevent complications and guide timely treatment.
Common Causes of a Painful Hard Vein in Leg
Several conditions can lead to a vein becoming hard and painful. Understanding the underlying cause is crucial, as it guides the right approach to care and helps prevent complications. The causes range from relatively minor issues to more serious vascular conditions, so paying attention to the specific signs and symptoms can make all the difference.
1. Superficial Thrombophlebitis
One of the most common reasons for a painful hard vein in leg is superficial thrombophlebitis. This condition occurs when a blood clot forms in a vein just beneath the skin, leading to inflammation. While it is generally less dangerous than a deep vein clot, it can still cause noticeable discomfort and warrants professional evaluation.
Superficial thrombophlebitis symptoms often include:
-
Pain or tenderness along the course of the affected vein
-
Redness or warmth over the vein
-
A firm, rope-like structure palpable under the skin
-
Mild swelling around the area
Although this condition is usually not life-threatening, it should be assessed by a healthcare professional. Early evaluation helps rule out more serious clotting disorders or the rare possibility of clot extension toward deeper veins. Additionally, timely care can alleviate discomfort and prevent the condition from worsening.
2. Varicose Veins
Another frequent cause of a hard and painful vein is varicose veins. Over time, weakened vein walls and valves can cause veins to enlarge and twist. In some cases, these veins become inflamed, resulting in tenderness or a firm, sore vein in the leg.
Key signs of inflamed varicose veins include:
-
Enlarged, twisted veins visible under the skin
-
Localized tenderness or aching, often worsening after prolonged standing
-
Mild swelling or a sensation of heaviness in the leg
Because inflamed varicose veins can mimic superficial thrombophlebitis, consulting a vein specialist is important. A proper assessment ensures the correct treatment and reduces the risk of further complications.
3. Injury or Trauma
A direct injury to the leg, such as a bump, bruise, or minor trauma, can also cause a vein to become hard and painful. While this is usually temporary, it can sometimes be confusing, especially if the vein appears unusually firm or swollen.
Symptoms of vein-related injury often include:
-
Localized bruising around the affected area
-
Tenderness along the course of the vein
-
Swelling or mild redness near the site of injury
Although minor trauma often resolves with rest, ice, and gentle elevation, persistent pain or unusual swelling should always be evaluated. Seeking professional guidance ensures that no underlying vein injury or clotting issue is missed.
4. Infection or Skin Inflammation
In certain cases, infection or skin inflammation can cause a vein to feel hard and tender. Conditions such as cellulitis, which is a bacterial infection of the skin and surrounding tissues, can affect areas near veins and lead to redness, warmth, and discomfort.
Signs to watch for include:
-
Red, warm, and tender skin over or near the vein
-
Fever, chills, or general feelings of illness
-
Rapidly spreading swelling or irritation
Prompt medical evaluation is essential for infections to prevent them from worsening. Early treatment with antibiotics and supportive care can reduce complications and improve recovery time.
When to Seek Medical Attention
Although some cases of a painful hard vein in leg may improve with rest, compression, or home care, it is important to recognize warning signs that require prompt evaluation. Ignoring these symptoms can allow underlying conditions to worsen, making early assessment by a healthcare professional crucial.
Seek medical attention if you notice any of the following:
-
Sudden, severe pain or swelling: A rapid onset of discomfort or enlargement in the leg could indicate a clot or acute inflammation that needs immediate evaluation.
-
Redness, warmth, or tenderness that spreads quickly: Expanding inflammation may signal infection or progression of thrombophlebitis, requiring professional care.
-
Fever or other signs of infection: When a hard vein is accompanied by fever, chills, or general malaise, it could point to a bacterial infection that must be treated promptly.
-
Swelling in both legs: While a single hard vein usually points to a localized problem, swelling in both legs can indicate deeper or systemic vascular issues that need attention.
-
Persistent hard vein: If the vein remains firm, painful, or tender for several days without improvement, it is important to have it evaluated by a vein specialist.
Consulting a vein specialist not only ensures an accurate diagnosis but also provides targeted treatment. Through careful assessment and advanced imaging, specialists can identify the underlying cause, manage symptoms effectively, and prevent potential complications. Early evaluation can also lead to faster relief, reduced discomfort, and better long-term vein health.
How Vein Specialists Evaluate a Painful Hard Vein
A vein specialist can determine the cause of a hard vein under skin and provide the most appropriate care. Evaluation typically involves:
1. Medical History Review
-
Past vein issues or blood clots
-
Recent injuries or trauma
-
Medications and lifestyle factors
-
Family history of vascular problems
2. Physical Examination
-
Examining the vein for firmness, redness, or swelling
-
Checking circulation and skin changes
-
Comparing both legs for asymmetry
3. Diagnostic Tests
-
Ultrasound (Doppler): Detects clots in superficial or deep veins
-
Blood tests: Assess clotting risk or infection markers
-
Imaging: Occasionally used for complex cases
Treatment Options for Hard Veins
Treatment varies depending on the underlying cause but generally focuses on reducing pain, inflammation, and preventing complications.
1. Conservative Measures
-
Compression therapy: Improves circulation and reduces discomfort
-
Elevation: Raising the leg above heart level several times a day
-
Pain relief: Over-the-counter anti-inflammatory medications
-
Activity modification: Avoid prolonged standing or heavy lifting
2. Medical Interventions
-
Minimally invasive procedures: For varicose veins or recurring thrombophlebitis
-
Anticoagulants: Rarely used if clot risk is higher
-
Antibiotics: Prescribed if infection is suspected
3. Lifestyle Steps
-
Maintain healthy weight to reduce vein pressure
-
Stay active with walking or low-impact exercise
-
Avoid smoking, which can worsen vein health
-
Monitor veins regularly for changes in appearance or tenderness
Preventing Hard Veins and Thrombophlebitis
Preventive measures can reduce the risk of painful veins and inflammation:
-
Wear compression stockings during long periods of sitting or standing
-
Elevate legs during rest
-
Maintain hydration to support healthy circulation
-
Regularly move and stretch to prevent blood pooling
-
Treat minor varicose veins before they become inflamed
FAQs About Painful Hard Veins
1. Can a hard vein under skin go away on its own?
Mild cases may improve with rest and compression, but persistent pain should be evaluated.
2. How can I tell if a tender vein in leg is serious?
Seek care if swelling, redness, warmth, or sudden pain occurs, especially if it spreads.
3. Is superficial thrombophlebitis dangerous?
It is usually not life-threatening but can rarely extend to deeper veins, requiring specialist care.
4. Can varicose veins cause painful hard veins?
Yes, inflamed varicose veins can become tender and firm, mimicking thrombophlebitis.
5. What treatments are most effective for a painful hard vein in leg?
Compression, elevation, anti-inflammatory medications, and evaluation by a vein specialist offer the best results.
Final Thoughts
A painful hard vein in leg can be uncomfortable and concerning. Understanding the potential causes, from superficial thrombophlebitis to varicose veins or injury, helps guide proper care. Early evaluation by a vein specialist ensures accurate diagnosis, effective treatment, and relief from discomfort. With targeted care, patients can prevent complications, protect vein health, and maintain active, healthy legs.
Vein specialists in Houston can provide expert care for hard veins, including advanced imaging, minimally invasive treatments, and personalized management plans. Consulting a local vein expert offers peace of mind and ensures the safest, most effective treatment for leg vein health.
Medical Disclaimer: This content is for educational purposes only and does not replace professional medical advice. Always consult a qualified healthcare provider for personalized diagnosis and treatment.